Pending review. Contribute to this article.
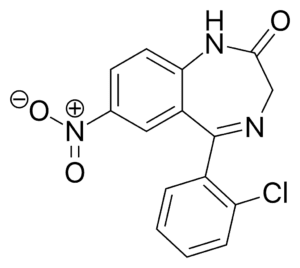
Clonazepam, sold under the brand name Klonopin among others, is a medication used to prevent and treat seizures, panic disorder, and the movement disorder known as akathisia. It is a tranquilizer of the benzodiazepine class. It is taken by mouth. It begins having an effect within an hour and lasts between 6 and 12 hours.
Common side effects include sleepiness, poor coordination, and agitation. Long-term use may result in tolerance, dependence, and withdrawal symptoms if stopped abruptly. Dependence occurs in one-third of people who take clonazepam for longer than four weeks. There is an increased risk of suicide, particularly in people who are already depressed. If used during pregnancy it may result in harm to the baby. Clonazepam binds to GABAA receptors, thus increasing the effect of the chief inhibitory neurotransmitter γ-aminobutyric acid (GABA).
Clonazepam was patented in 1960 and went on sale in 1975 in the United States from Roche. It is available as a generic medication. The wholesale cost in the developing world is between US$0.01 and US$0.07 per pill. In the United States, the pills are about US$0.40 each. In 2016 it was the 42nd most prescribed medication in the United States with more than 18 million prescriptions. In many areas of the world it is commonly used as a recreational drug.
Protracted withdrawal
Protracted withdrawal applies to signs that linger until the end of acute withdrawal. Patients who have abused Klonopin and have taken very high doses of the medication that experience longer withdrawal times.
Individuals may feel a general malaise, cravings, anxiety, depressive symptoms. Some somatic symptoms, such as nausea, lightheadedness, headache, mild fever or chills, and so on, may continue to occur. A further period of rebound anxiety may also occur near the end of this stage.
There is a portion of the literature on opioid withdrawal in general, including Klonopin and other benzodiazepines, which explains the third phase of withdrawal, which consists mostly of psychological symptoms such as mood swings, periods of irritability, periods of anhedonia (difficulty feeling pleasure) and depressive symptoms that tend to occur in the body. This post-acute withdrawal syndrome (PAWS) is not generally recognized as a stage of withdrawal by other experts, nor is it officially mentioned in the Diagnostic and Statistical Manual of Mental Disorders of the American Psychiatric Association; however, it is acknowledged as valid by some individuals in the field of addiction.
This is suggested that people who do not have PAWS symptoms treated are at higher risk of relapse.
Medications used to help in the removal of Klonopin
Withdrawal from benzodiazepine, such as Klonopin, can be potentially dangerous due to the possibility of seizures (though this possibility is rare).
As a consequence, therapeutic detoxification is often necessary for the removal of benzodiazepine. Several medications can be used to assist with the withdrawal process, including:
- Selective serotonin reuptake inhibitors, such as Paxil and Prozac, can be useful in treating some of the effects of Klonopin withdrawal.
When a patient has complications such as seizures, doctors may use anticonvulsant drugs (e.g., Tegretol or carbamazepine to manage seizures).
Some of these anticonvulsants can also aid with the withdrawal process linked to the discontinuation of Klonopin.
The melatonin hormone has been beneficial in helping individuals who experience insomnia during the withdrawal process.
Melatonin is a hormone that causes sleep. Many signs of Klonopin withdrawal and reversal of tolerance can also be treated.
Any number of medications can be used to treat particular symptoms during the withdrawal period.
Research suggests that the most successful way of controlling withdrawal from benzodiazepines, such as Klonopin, is to implement a tapering mechanism where the patient in withdrawal continues to obtain progressively smaller doses of the medication before the formal withdrawal.
Beyond Detox
After an individual is considered to be physically stable, the emotional side effects of withdrawal are discussed more thoroughly.
Cognitive Behavioral Therapy ( CBT) and Motivational Interview (MI) are two types of therapy that can be used during benzodiazepine addiction care.
Individuals also attend both group and individual CBT sessions, which can often include research and instructional sessions aimed at discovering the root of addiction and preventing potential stressors and causes in the potential.
MI can help increase the level of internal motivation of an individual by offering rewards for clean drug testing. Peer and family support networks are also essential components of a holistic system for treating opioid addiction.
Care standards can change during withdrawal as the individual needs and circumstances change.
Relapse is typical in individuals who are addicted to benzodiazepines and are particularly dangerous after detoxification.
Someone who has been used to using drugs at a certain amount, but has not used them for a while, and then returns to previous rates of use, may end up suffering from a fatal overdose.
The National Institute for Drug Abuse ( NIDA) registered a fourfold rise in benzodiazepine overdose deaths from 2001-13 to almost 7,000 deaths in 2013.
A relapse may occur as someone tries to self-medicate what may be uncomfortable symptoms of withdrawal.
Therapy and psychological help during benzodiazepine withdrawal are essential to reduce and prevent future relapse and avoid catastrophic consequences.
Clonazepam withdrawal is best handled by incorporating both pharmacological and clinical approaches, beginning with natural detoxification.
- Inside The Fragmented Minds of People With Dissociative Identity Disorder
- Power Foods for the Brain Protracted withdrawal
This refers to the symptoms that persist after acute withdrawal ends. People who abuse Klonopin and were taking extremely high doses of the drug may experience more extended periods of withdrawal.
Individuals will experience general feelings of malaise, cravings, anxiety, depressive symptoms, and may continue to experience some somatic symptoms, such as nausea, lightheadedness, headache, mild fever or chills, and so forth. An additional period of rebound anxiety may also occur near the end of this stage.
There is a section of the literature regarding withdrawal from drugs in general, including Klonopin and other benzodiazepines, that describes a third phase of withdrawal that consists primarily of psychological symptoms, such as mood swings, periods of irritability, periods of anhedonia (difficulty experiencing pleasure), and depressive symptoms that continue to present themselves on an intermittent basis for weeks to years following discontinuation of the drug of choice. This post-acute withdrawal syndrome (PAWS) is not universally accepted as a stage of withdrawal by many researchers, nor is it formally listed in the American Psychiatric Association’s Diagnostic and Statistical Manual of Mental Disorders; however, the syndrome is accepted by some individuals in the field of addiction as legitimate.
It is suggested that individuals who do not have the symptoms of PAWS addressed are at a higher risk for relapse.
Medications Used to Assist with Withdrawal from Klonopin
Withdrawal from a benzodiazepine such as Klonopin can be potentially fatal due to the risk for seizures (although this risk is rare).
As a result, medical detox is always necessary for benzodiazepine withdrawal. Several medications can be used to assist in the withdrawal process, including:
Selective serotonin reuptake inhibitors, such as Paxil and Prozac, may be useful in addressing some of the symptoms of Klonopin withdrawal.
If an individual develops complications, such as seizures, physicians will use anticonvulsant medications (e.g., Tegretol or carbamazepine to control the seizures). Some of these anticonvulsants may also assist with the withdrawal process related to discontinuation of Klonopin.
The hormone melatonin has been useful in assisting individuals who develop insomnia during the withdrawal process. Melatonin is a hormone that induces sleep. It also may address other symptoms of Klonopin withdrawal and reverse tolerance.
Any number of medications could conceivably be used to address specific symptoms during the withdrawal process. However, research indicates that using a tapering process, where the individual in withdrawal continues to receive increasingly smaller dosages of the drug until formal discontinuation, is the most effective means to manage withdrawal from benzodiazepines such as Klonopin.
Beyond Detox
After an individual is deemed physically stable, the emotional side effects of withdrawal are considered more thoroughly. Cognitive Behavioral Therapy (CBT) and Motivational Interviewing (MI) are two forms of therapy that may be used during benzodiazepine addiction treatment. Individuals often attend both group and individual CBT sessions, which may also include homework and educational sessions that strive to find the cause of addiction and how to avoid future stressors and triggers in the future. MI can aid in increasing an individual’s internal motivation level by offering rewards for clean drug tests. Peer and family support groups are also useful aspects of a comprehensive substance abuse treatment program. Levels of care may change throughout withdrawal as individual needs and circumstances change as well.
Relapse is common in individuals addicted to benzodiazepines, and it is especially hazardous after detox. Someone who has been accustomed to using drugs at a certain level, but has not used them for a period of time and then returns to previous use levels, may end up suffering a fatal overdose. The National Institute on Drug Abuse (NIDA) reported that benzodiazepine overdose deaths increased fourfold from 2001-2013, to close to 7,000 fatalities in 2013.
A relapse may occur as someone strives to self-medicate what may be uncomfortable withdrawal symptoms.
Therapy and psychological support are vitally important during benzodiazepine withdrawal in order to reduce and minimize potential relapse and avoid tragic consequences.
Clonazepam withdrawal is best managed with a combination of both pharmacological and therapeutic methods starting with medical detox.
